ASB in Blood Cultures (2): Clostridia
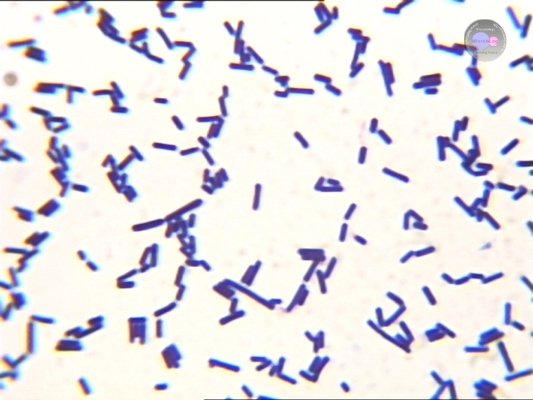
Submitted by amh10 on 1 October, 2006 - 16:13 · Bacteriology Microbiology: · Clostridium is latin for "little splindle". · Gm+. Is Gm variable and can be Gm-.
· Spore forming anaerobic bacilli. · Large, straight or slightly curved roads with rounded ends. Pleomorphic morphology. · Most are saprophytes, occuring in soil, water and decomposing matter. Important in the process of putrefaction. · C. perfringens, C. septicum & C. novyi causes gas gangrene and other infections. · C. tetani causes tetanus. · C. botulinum causes botulism. · C. difficile causes pseudomembranous colitis and antibiotic associated diarrhoea. · Most of the species are highly toxinogenic. Clostridium perfringens: · Capsulate, non-motile. · Rapidly growing (doubling time ~8min), especially @ 42 C.
· Nagler reaction: o C. perfringens phospholipase causes turbidity around the colonies on egg-yolk medium. Inhibited by specific antiserum. o Food poisoning strains produce heat resistant spores, whilst the type A spores producing gas gangrene are inactivated by heat quickly.
· C. perfringens is the commonest cause of gas ganrene. Rapidly spreading oedema, myositis, tissue necrosis and production of gas. Clinical diagnosis with laboratory diagnosis. Causes of infection include soil contaminated wounds, street dust and dirty clothing. Skin contaminated with intestinal contents may sometimes carry the spores. · Anaerobic coniditions occur in the face of ischaemia, and together with dead tissue and pyrogenic toxins promote gas gasgrene. In these conditions rapid multiplication of the organism and the production of a range of toxins and agressions accelerated disease. o Hyaluronidase produced by C. perfringens breaks down the intraceullar cytoskeleton. o Collagenase and other proteinases break down muscles and liquiefy. o alpha-toxin causes the widespread toxiaemia. · C. perfringens has been implicated in the following infections: o Puerperal infections: for faecally contamination of the perineum -> fulminant pelvic infection & DIC. o Peritoneal infections: perforated appendix/SBO. o Contaminated adrenaline injections. o Prolonged anoxia of limbs during surgery. o NB: Clostridia may be isolated in small numbers from wound which do not clinically look like gas gangrene, therefore results should be interpreted in clinical context. These include: crepitus, a sponge like consistency, local pain and swelling. When the patient becomes toxaemic, they can be comatose. · Laboratory diagnosis: o Sloughs of necrotic tissue should be Gm stained. o Direct smears of wounds will give an indication of bacterial role and the possibilty of contamination. · Treatment: o Removal of sutures, debridement, fasciotomy, removal of foriegn bodies, with any surgical sites left open. o Antimicrobials should cover GPCs, coliforms and anaerobes: penicillin, metronidazole and gentamicin. Consider clindamycin and gentamicin or a cabapenem. ICU care as required. o Some contraversial roles for hyperbaric oxygen limiting tissue necrosis. · Prophylaxis: o Surgical wounds: Prolonged topical treatment (1-2 days) povidone-iodine can be used in orthopaedic cases. If inevitable skin contamination occurs together with skin devitalisation there is a role for peri-operative penicillin. o Accidental wounds: Those wounds that have been contaminated by soil, clothing and other foreign bodies (risk of anaerobes) and other situations where foreign bodies are driven into devitalised tissue (gunshots & RTAs). Some believe that there is a role for prohylactic benzylpenicillin. · C. perfringens food poisoning: o Large numbers of viable oragnisms much be ingested to produce clinical disease. o The syndrome is mediated by an enterotoxin that is released when sporulation occurs in the gut. o Abdominal cramps 8-12 hr spot ingestion followed by diarrhoea. Fever and vomiting do not usually occur and the symptoms resolve within 1-2 days. No treatment is required. A carrier state exsists for several weeks, although this would not prevent return to work. o Infection occurs through cooked meat that has been allowed to stand at room temperature, as some strains are heat resistant. The heat sensitive type-A strains may also result in infection if the food is innoculated during the cooling period. o Laboratory diagnosis involves isolation of similar strains in large numbers from food sources and faeces. o Causes of food poisoning: 1. Campylobacter spp. 2. Salmonella serotypes. 3. Staphylococcus aureus. 4. C. perfringens. · C. perfringens colitis: o Sporadic diarrhoeal syndrome occuring the elderly after antibiotic treatment. An enterotoxin exhibiting a cytopathic effect can be isolated from the faeces. o Enteritis necroticans occurs when the enterotoxin in the gut combines with a proteinase inhibitor (the beta-toxin from sweet potato) to produce a necrotizing enteritis. Clostridium septicum: · Readily formed spores allow changes in the appearance: Gm+ "citron bodies"; ranging to central or sub-terminal bulging spores. · Actively motile with peritrichous flagellae. · Grows well @ 37 C on normal media. · Irregular, transparent and droplet like surface colonies, greyish and opaque. The projecting radiations are coarser than those of C. tetani. · This is one of the gas ganrene clostridia. Bacteraemia occurs duing mucositis, and neutropaenia predisposed patients to gas ganrene. Typhilitis is a rapidly fatal terminal ileal infection and sepsis ocurring in the immunocompromised. · Laboratory diagnosis involves the IM injection of cultures into mice resulting in a rapidly spreading oedema with gas formation, resulting in death in less than 2 days. Out of the four toxins produced (alpha, beta, delta and epsilon), alpha toxin is necrotizing and haemolytic. This is different from the alpha toxin of C. perfringes as it does not have phospholipase C. · C. septicum can be found in animal intestines and soil. Clostridium novyi: · Morphologically similar to C. perfringes. Readily killed when the vegetative state is exposed to the air. Out of the four types (A,B, C & D), type A is the most medically relevant, causing gas gangrene in IVDUs. Clostridium sporogenes: · Gm+ motile bacillus widely distributed in nature. · It may be encountered in the lab in mixed cultures.
· Very heat resistant spores. · It is considered benign and non-pathogenic, but may enhace local conditions. Clostridium tetani: · Gm+, but may appear Gm-. · Fully developed terminal spore gives a drumsrick appearance. · Obligate anaerobe, motile via peritrichous flagellae. · A thin film is produced on enriched blood agar.
· Highly resistant spores, but glutaraldehyde is effective. · Toxins: o tetanolysin - oxygen labile haemolysin. o tetanospasmin - neuro muscular pathogenic effect. § Gene encoded on a 75kb plasmid. The toxin is synthesised as a single polypeptide (150kDa), which undergoes post translational cleavage (heavy & light chain linked by a disuplhide bridge). Tiny lethal dose required, but only effective in humans parentrally (not oral). o Bacilli remain at the site of infection, toxin causes localized or generalized tetanus. Spread is haematogenous. The heavy chain mediates attachment to gangliosides and internalization of the toxin. Through retrograde axonal transport and trans-synaptic spread, the toxin affects the cranial nerves first as these are the shortest. Once internalized, the light chain disrupts the synpatic vesicle membrane. Prevention of GABA results in a sustained state of excitatory discharge -> motor spasms. · Tetanus bacilli are found in animinal faeces and soil (especially manure), from where they get into the human intestine. The spores are everywhere in the environment. Infection may occur through superficial grazes and garderners are especially at risk. · Pathogenesis: o Germination requires reduced oxygen tensions as well as the materials of devitalized tissue. Infection is promoted by simultaneous growth of facultative anaerobes. o Otogenic tetanus: the EAM is the site of infection, through aggressive ear cleaning. o Cryptogenic tetanus: source unknown. o Tetanus neonatorum: treatment of the umbillical cord stump with primitive turd-containing preparations. Fatality rate >50%. o Post-op tetanus: previously due to partially sterilized catgut, gloves etc. · Clinical features: o Gradual onset. o Pain & stiffness near the wound. o Lockjaw. o Sardonic grin. o Opisthotonos (extreme arching of the back). o 10-14 days between the injury and the onset of symptoms. o Sweating, tachycardia, arrhythmia and autonomic instability are poor prognostic signs. o Highest incidence in devloping countries, associated with a fertile soil and warm climate. Previous association with non-sterile ear piercing. · Treatment: o Paralysis and ventilation until the toxin has decayed (several weeks). o 10 000U of human tetanus Ig (slow IV injection). o Wound exploration, debridement, with any surgical sites left open. o Penicillin or metronidazole with the HTIg. · Laboratory Diagnosis: o Gram stains of wound smears: don't often proove useful! o Direct culture on blood agar heated anerobically. Material from wounds is heated at various temperatures for varying time to exclude non-sporing bacteria. o An anaerobically prepared culture may be injected into mice, with control mice protected by antitoxin. · Prevention and Control: o Adequate wound toilet and proper debridement. o Specific prophylaxis for the non-immunized patient: § deep wound § puncture or stab wound § a wound with a lot of bruising and devitalised tissue § a septic wound § a heavily contaminated wound. o Adsobed tetanus toxoid: immune for 6 months after a single shot, or 5-10 years are a three shot course. After this time, the patient should be regarded as non-immune. o Passive immunization with antitoxin (HTIg): prophylactic dose: 250-500U. o Combined active-passive immunization: patient recieve the toxoid at the same time as the HTIg. The full course of toxoid should be completed. o If there is a significant risk of infection, penicillin or clindamycin should be used. Clostridium botulinum: · Strictly anaerobic Gm+ bacillus. · Motile with peritrichous flagella, oval subterminal spores. · Widley distributed saprophyte: soil, manure, fruits, veg. · Optimum growth @35 C, some strains grow and produce toxin @1-5 C. · Potent food neurotoxin. In all sorts of food from sausages to honey. Fodd may not look spoilt. The preformed protein (resistant to proteolytic enzymes) is absorbed through the GI tract. · Highly resistant spores (can survive 100 C for several hours), can be killed by moist heat 120C for 5 mins. · Problems occur in canning factories where the contents of the can are not adequately heated. The spores survive radiation. · Toxins: o Seven main types of toxin of C. botulinum: A-G. These are antigenically different but pharmacologically identical. A, B & E are most common. Only type-specific antitoxin is effective. o Type A&B - soil source,type E - marine source. o The toxin binds irreversibly to the presynaptic nerve endings, where ACh release is inhibited. · Clinical features: o Symptoms may develop after 1-2 days of ingestion. Initial nausea & vomiting. o Oculomotor palsy, ptosis, vertigo and diplopia. o Pure descending motor paralysis. No LOC/sensory loss. Progressive thirst (dry mouth and tongue), following by dysphagia, dyspnoea and abdo pain. o Death due to cardiac/respiratory failure. o Rarley wound infection by C. botulinum leads to botulism. o Floppy child syndrome: Children <6 months developed a flaccid paralysis due to toxin production in the gut. This occurs because gut colonization resistance is poor. It has been attributed to the presence of C. botulinum spores in honey given to babies with the feed. · Laboratory diagnosis: o Refer to a reference lab: toxin maybe demonstrated by toxin-antitoxin neutralization test in mice. · Treatment: o Remove unabsorbed toxin from the stomach and GI tract. o Neutralize unfixed toxin by giving polyvalent antitoxin. o Give ICU care & support. · Control: o Of commercial food preparation. o Those who have had a suspected contact a prophylactic dose of polyvalent antitoxin should be given. Three doses of mixed toxoid can be given every 2 months to induce active immunity. Clostridium difficile: · Motile Gm+ rod with subterminal spores · Commensal in neonates and babies up to weaning age (no receptors), not adults. · Toxin A & toxin B enterotoxin ->pseudomembranous colitis. · Links to antibiotics - especially clindamycin, cephalosporins & carbapenems. · Laboratory diagnosis: ELISA for toxin A&B. · Treatment: take your pick(!). Metronidazole, then vancomycin (various doses, durations & regiemes). · Importance of infection control.
|